Symptoms of MRSA and Staph Infections
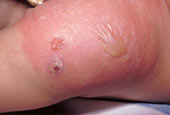
Cellulitis Staph infection. Symptoms are a deep red color and swelling. A vaccination was the cause of this infection. Photo credit: CDC/Mathies
The most common visible signs of MRSA and Staph are:
- Bumps, pimple-like lumps, or blisters on the skin, either singly or more than one. These are the most common outward signs of a Staph aureus or MRSA infection (see Staph vs MRSA).
- Swelling, reddening, and tenderness of the skin often surround the lumps or bumps.
- White or yellow pus filled heads are often found at the center of lumps, which often drain on their own.
- Skin infections on fingers, legs, arms, back, face or buttocks are most common, especially for infections caught in the community. Painful Staph nose infections are also very common (see “Is Staph living in your nose?”).
- Internal infections or surgical site infections are most common with hospital or healthcare acquired MRSA or Staph.
See how to recognize 6 types of Staph infection below, including folliculitis and boils. Also below are the key symptoms of more dangerous MRSA infections.
Does Staph infection itch?
Yes, Staph is often very itchy and can feel like your skin is crawling. Lumps, rashes and skin eruptions itch and can be tender and warm to the touch. Lumps can sometimes become deep sores with increasing pain and swelling if left unchecked. The color of the surrounding skin area is often red to purple and may begin to spread as the infection progresses.
6 common signs of Staph and MRSA skin infections
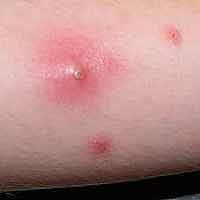 Boils – Boils are bumps with a pus filled head that are usually small and superficial near the surface of the skin. If boils enlarge and grow together, they can form a multi-headed lump called a carbuncle. It is important that you do not try to lance or drain these on your own as you can push the infection inside your body. Boils are often treated by lancing and draining (by a doctor) and may include a course of antibiotics.
Boils – Boils are bumps with a pus filled head that are usually small and superficial near the surface of the skin. If boils enlarge and grow together, they can form a multi-headed lump called a carbuncle. It is important that you do not try to lance or drain these on your own as you can push the infection inside your body. Boils are often treated by lancing and draining (by a doctor) and may include a course of antibiotics.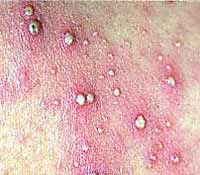 Folliculitis – Similar to boils, folliculitis is a deep infection of a hair follicle, forming bumps usually less than a quarter inch in diameter, often surrounded by an area of inflamed red or pink skin. Folliculitis usually forms white heads that can occur anywhere on the skin. The areas affected are often itchy and sometimes painful.
Folliculitis – Similar to boils, folliculitis is a deep infection of a hair follicle, forming bumps usually less than a quarter inch in diameter, often surrounded by an area of inflamed red or pink skin. Folliculitis usually forms white heads that can occur anywhere on the skin. The areas affected are often itchy and sometimes painful.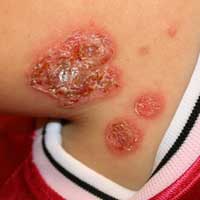 Impetigo – Impetigo looks like crusty oozing bumps, blisters or lesions, usually yellow to red in color, that break open easily. These crusty scabs are made of dried blood serum and are most common on the face, legs and arms. Impetigo is common on the face and can spread easily to other parts of the body. Impetigo is more common in children than adults.
Impetigo – Impetigo looks like crusty oozing bumps, blisters or lesions, usually yellow to red in color, that break open easily. These crusty scabs are made of dried blood serum and are most common on the face, legs and arms. Impetigo is common on the face and can spread easily to other parts of the body. Impetigo is more common in children than adults.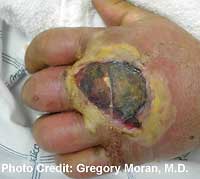 Abscess – Abscesses are pus filled cavities that form deep under the skin that rarely have a head or drain on their own. You can sometimes feel the fluid inside of an abscess if you press on it with your fingers. It is important that you do not try to lance or drain these on your own as you can push the infection deeper into your body. A boil is a small, shallow abscess.
Abscess – Abscesses are pus filled cavities that form deep under the skin that rarely have a head or drain on their own. You can sometimes feel the fluid inside of an abscess if you press on it with your fingers. It is important that you do not try to lance or drain these on your own as you can push the infection deeper into your body. A boil is a small, shallow abscess.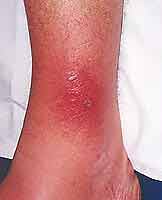 Cellulitis – Cellulitis is a deeper and more serious infection with significant swelling and tenderness. It has a deep red color and often increases size as the infection grows (doctors will often draw a line around it to determine if it’s growing or shrinking). Sometimes red streaks may radiate out from the center. Bumps and blisters may or may not be present with cellulitis. This condition normally begins when infecting bacteria enter a break or cut in the skin. Cellulitis is most common on the lower legs, but can also be on the arms, hands and face. The elderly and people with a compromised immune systems are at a higher risk for this condition.
Cellulitis – Cellulitis is a deeper and more serious infection with significant swelling and tenderness. It has a deep red color and often increases size as the infection grows (doctors will often draw a line around it to determine if it’s growing or shrinking). Sometimes red streaks may radiate out from the center. Bumps and blisters may or may not be present with cellulitis. This condition normally begins when infecting bacteria enter a break or cut in the skin. Cellulitis is most common on the lower legs, but can also be on the arms, hands and face. The elderly and people with a compromised immune systems are at a higher risk for this condition.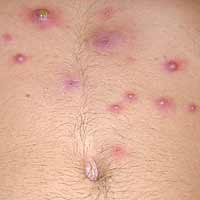 Furunculosis – Hair follicles that become infected deeper in the tissues, with swelling and red skin (also called boils). If the abscesses are larger than boils, or if there are multiple boils, the condition is usually called a carbuncle.
Furunculosis – Hair follicles that become infected deeper in the tissues, with swelling and red skin (also called boils). If the abscesses are larger than boils, or if there are multiple boils, the condition is usually called a carbuncle.
Can you diagnose Staph or MRSA based on symptoms?
Symptoms alone are not enough to tell if you have Staph or MRSA. Only a professional test can confirm if you have a MRSA infection or Staph (or another type of infection). So use these signs and symptoms as a helpful guide, but not as a substitute for getting tested by your doctor.
If you think you could be infected, consider seeing your doctor as soon as possible. Be aware that MRSA and Staph are commonly misdiagnosed as bug or spider bites. Avoid puncturing any pus filled heads yourself – incising and draining should only be performed by a healthcare professional to prevent the infection from spreading or growing worse.
Where do Staph skin infections usually show up?
These infections can show up anyplace on your body but are more common in the following specific areas.
- Areas of clothing friction and irritation, such as the legs, buttocks and shaving areas
- Sweaty areas like armpits, neck, face, groin and feet

Staph versus MRSA symptoms
Because MRSA is a specific type of Staph bacteria, both infections share many of the same signs or characteristics. However, MRSA superbug infections differ from Staph infections in that MRSA bacteria have learned to adapt to many types of antibiotics (see more about antibiotics for MRSA), making them more virulent.
In addition to the signs above, you may have MRSA if:
- There is minimal or no improvement after taking antibiotics for 2 to 3 days.
- You have rapid spreading of your infection
- You have a prior history of MRSA infections
- If you’ve used antibiotics multiple times
- You are a carrier of MRSA either in your nose or on your body
If you think you are infected, consider visiting with your doctor or an infectious disease specialist (an I.D. doctor) to get a Staph or MRSA culture test to confirm what is causing your condition.

See our PRIVACY POLICY
More serious symptoms of a MRSA infection
Most infections caused by MRSA and Staph are limited to the skin. However, Staph can also enter your bloodstream and spread to internal organs. More severe indicators of internal infection include:
- Fever
- Chills
- Weakness or fatigue
- Shortness of breath
- Rashes
- Headache
- Muscle aches
- Nausea
- Acute pain
If you show signs of a skin infection and have any of the above symptoms, see a doctor as soon as possible. The following serious conditions can occur with internal Staph or MRSA:
- Staphylococcal pneumonia – Abscess formation in the lungs. An underlying lung disease is the usual precursor.
- Pnuemonia – pneumonia caused by MRSA or Staph bacteria.
- Endocarditis – Infection of the heart valves that can lead to heart failure.
- Osteomyelitis – Infection of the bones that causes severe inflammation.
- Staphylococcal sepsis – A widespread infection in the bloodstream that can lead to shock, circulatory collapse and death. People with large areas of severe burns are particularly susceptible.

- Find out what you Doctor probably won’t tell you about your infection.
- How do Staph and MRSA spread to others?
- 7 myths and little known facts about MRSA.
How to Win the Infection BattleMRSA and Staph are serious and potentially life-threatening infections. Antibiotics and conventional medicine often fail against these superbugs. Fortunately, there are powerful natural and alternative remedies for handling these infections.
The MRSA Secrets Revealed Program contains Michelle’s 3-Step Infection-Free Method™, a complete how-to guide to stop these infections. It includes the strongest remedies for skin, internal, nose and other types of infection. Tools for making antibiotics work better with less side effects are provided. The program also includes ways you can protect yourself and your family in hospitals and in the community.
Get started now by clicking the button below.









