MRSA Antibiotic Treatment Overview
Antibiotics are commonly prescribed as a treatment for MRSA skin infections, either by themselves or along with draining of the infection by a healthcare professional.
Antibiotics are also the standard medical therapy for internal MRSA infections. Antibiotic therapy is often prescribed for the following types of infections:
- Skin infections, such as boils or abscesses, that do not respond to incision and drainage
- Systemic or internal infections such as bone, implant or lung infections
- Severe local symptoms
- Severe internal infections that require surgery to remove infected areas
- Immunosuppressed or immune-compromised people
Because MRSA is becoming more resistant, and it’s more common for antibiotic treatments to fail, and treatment may require the use of newer antibiotics, such as the “glycopeptides” which includes Vancomycin and Zyvox. Unfortunately, there are newer strains of MRSA that are becoming resistant to these two drugs. When it comes to antibiotics, the list of what works for MRSA is growing shorter each year.
It’s common for doctors to not tell you about the many antibiotic side effects (more below), and what to expect when it comes to dealing with MRSA (read here for more). There are also alternative treatments available which can be used alone or in conjunction with antibiotics to help improve your chance of success.
Top 5 MRSA antibiotic therapies for skin infections
MRSA is now resistant to many types of antibiotics.
Below are the five commonly prescribed antibiotics for MRSA skin infections, which are commonly picked up in communities as community type MRSA or CA-MRSA.
1. Clindamycin
It has been successfully and widely used for the treatment of soft tissue and skin infections as well as bone, joint and abscesses caused by Staph and MRSA. MRSA is becoming increasingly resistant to clindamycin in the United States.
- Resistance: MRSA is becoming increasingly resistant to clindamycin in the United States.
- Side Effects and Precautions: Diarrhea is the most common side effect, and it can promote C. difficile overgrowth infections in the colon. C. difficile infections appear to occur more frequently with clindamycin than other antibiotics. Other side-effects are pseudomembranous colitis, nausea, vomiting, abdominal cramps, skin rashes and more.
2. Linezolid (Brand Names: Zyvox, Zyvoxid or Zyvoxam)
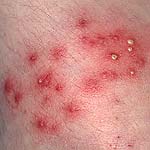
Folliculitis is a common type of MRSA skin infection often treated with oral antibiotics.
Approved for use in the year 2000, Linezolid is FDA approved for treating soft tissue and skin infections, including those caused by MRSA. It is often prescribed for CA-MRSA pneumonia and in particular, HA-MRSA pneumonia. It’s commonly prescribed to people of all ages and is one of the most expensive treatment options, for a single course costing upwards of $1-2,000 for 20 tablets.
- Resistance: To minimize resistance, this is a “last resort” antibiotic and is not usually prescribed unless Vancomycin or other antibiotics don’t work.
- Side Effects and Precautions: Common adverse events when used for short durations are: diarrhea, vomiting, headache, dizziness, and nausea. Long-term use has led to serious effects including bone marrow suppression, myelosupression, low platelet counts, peripheral neuropathy, optic nerve damage and lactic acidosis. It’s also associated with C. difficile infections in the colon.
3. Mupirocin (Brand Name: Bactroban)
Commonly used as a topical cream for minor skin infections and skin lesions for Staph aureus, MRSA and Streptococcus infections. Mupirocin ointment is applied to reduce or eliminate MRSA colonization in the nose (see also “MRSA carriers”). It’s commonly used before surgical procedures to help prevent the surgical site from becoming infected with MRSA. It is commonly prescribed for children and adults and there is limited safety data for pregnant and nursing mothers.
- Resistance: It has been reported that MRSA resistance to mupirocin is occurring in some communities.
- Side Effects and Precautions: Possible side effects include headache, rash and nausea as well as burning, dizziness and secondary wound infection. Like other antibiotics, prolonged use may result in overgrowth of bacteria that are not susceptible to it, as well as an overgrowth of fungal organisms (such as yeast infections).
4. Trimethoprim-Sulfamethoxazole (Brand Name: Septra or Bactrim)
It is not FDA-approved for the treatment of Staphylococcal infections (including MRSA). However, laboratory tests have shown most CA-MRSA strains are susceptible and so this drug has become a treatment option for Staph and MRSA. It is commonly used for skin and wound infections, urinary tract infections, lung infections, ear infections, septicemia, and other types of infections.
- Side Effects and Precautions: Not recommended for women in their third trimester of pregnancy or infants less than 2 months old. Side effects can include mild allergic reactions, fever, sore throat, skin rashes, cough, diarrhea, and serious adverse effects can include myelosupression, acute renal failure, severe liver damage and more.
5. Tetracyclines (Doxycycline and Minocycline)
Data suggests these drugs are effective in treatment of soft tissue and skin infections, but not for deeper or more severe infections.
- Side Effects and Precautions: Not recommended during pregnancy or lactation. Not recommended for children under 8 years old because of potential decreased bone growth and tooth discoloration. Doxycycline side effects can include an increased risk of sunburn when exposed to sunlight, diarrhea, and allergic reactions. Minocycline side effects can include risk of sunburn (like doxycycline), upset stomach, diarrhea, dizziness, headache, tinnitus, vomiting, allergic reaction and more. Serious but rare side effects for minocycline can include fever, yellowing of the eyes or skin, vision changes and more
Top 4 antibiotic treatments for internal or severe infections
Hospitalized patients with more complicated or severe forms of infections are often prescribed one of the following four antibiotics. These infections can include deep soft-tissue infections, surgical infections, major abscesses, wound infections and burn patients.
Oftentimes a broad-spectrum antibiotic is used in conjunction with the following antibiotics. Most options below use intravenous methods of delivering antibiotics into the body. A picc line may be used for prolonged treatment.
1. Intravenous (IV) Vancomycin
Vancomycin is often called an antibiotic of last resort for MRSA, though resistance against it has been growing. Vancomycin requires IV administration into a vein and can occasionally have severe side effects. Duration of treatment can last weeks to months. Tissue penetration is variable and it has limited penetration into bone. It’s often prescribed for pneumonia (both HA-MRSA and CA-MRSA strains).
- Resistance: Some strains of MRSA are now becoming resistant to Vancomycin, with one strain called “VRSA” (Vancomycin resistant Staph aureus).
- Side Effects and Precautions: Serious side effects can include ringing in ears, diarrhea, and hearing problems. Like most antibiotics, it can cause secondary infections like thrush or yeast infections. Because this medication is eliminated through the kidneys, it could cause kidney problems in the elderly or those with impaired kidney function.
2. Oral or Intravenous (IV) Linezolid
See the skin infection above for more info.
3. Intravenous (IV) Daptomycin
Daptomycin is FDA approved for adults with Staph aureus bacteremia, some forms of endocarditis and some skin and soft tissue infections. The safety and efficacy of daptomycin in children have not yet been established.
4. Oral or Intravenous (IV) Clindamycin
See the skin and soft tissue infection section above for more info.
What’s the best antibiotic for MRSA?
Finding the right antibiotic. If you think you have MRSA, talk with your doctor about getting tested to help see which antibiotics could actually work against your particular infection – click here for more about testing.
What’s best for you? The antibiotic your doctor may prescribe can vary due to the location of your infection, severity, your health status and if you have allergies to any antibiotics. So keep in mind that the information on this page is not all-inclusive, nor is it meant to imply that any of these drugs are safe or effective options for you.
About side effects, drug interactions and things to avoid with these drugs. Many things can weaken the effects of some antibiotics, and some things don’t mix well with these drugs. You’ll get the most benefit from antibiotics by knowing how to use them properly, safely and effectively. The info on this page is abbreviated and does not include all possible side effects, interactions and contraindications. so be sure to talk with your doctor about your medications and look at the drug product insert for a complete listing side-effects, possible drug or food interactions and precautions.
Which antibiotics should you avoid?

MRSA is currently “immune” to the following types of antibiotics:
- Penicillin class antibiotics including: Methicillin, Penicillin, and Amoxicillin
- First generation Cephalosporins such as cefazolin, cephalothin and cephalexin. These are a Penicillin-like class of antibiotics and they may be used for non-resistant Staph aureus infections or mild cases of MRSA.
- Resistance has been growing in many other classes of antibiotics as well including Vancoymcin.
Per the CDC and other research studies, these antibiotics are not good choices because MRSA develops resistance to them quickly. Other options should be considered first:
- Fluoroquinolone class antibiotics such as ciprofloxacin (“Cipro”) and levofloxacin
- Macrolide class antibiotics such as erythromycin, clarithromycin and azithromycine.
Importantly, Fluoroquinolones can have very severe side-effects and have been associated with myelosuppression, temporary and permanent neuropathy (tingling and numbness) and lactic acidosis during prolonged therapy. They also have some of the highest risks for causing colonization with either MRSA or C. difficile.
Independent Side Effects Listing. RxISK.org is a free, independent drug safety website where you can research your antibiotic for ALL of the side effects that actual people are experiencing. You can also report your side-effects. Click here to go RxISK.org.
What other options are there?
Unfortunately, MRSA is constantly becoming more resistant to more antibiotics. I agree with the CDC who stated it is only a matter of time before antibiotics can no longer can be relied upon.
Additionally, antibiotics often make people so sick they are unwilling to go another round. May people have tried everything with no luck. Fortunately, there are alternative treatment choices that actually work for MRSA and have little or no side-effects.

References:
CDC outpatient management of MRSA skin infections:
www.cdc.gov/mrsa/pdf/Flowchart_pstr.pdf
Clinical Practice Guidelines by the Infectious Diseases Society of America for the Treatment of MRSA Infections in Adults and Children:
https://cid.oxfordjournals.org/content/early/2011/01/04/cid.ciq146.full








