Conventional Treatment Approaches
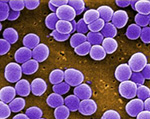
Staph aureus bacteria (above) started becoming resistant to antibiotics shortly after these drugs were discovered in the 1930’s.
In conventional, mainstream or western medicine, antibiotics are the primary choice for infection treatment of any kind. Conventional approaches may also include incision and draining (for skin infections), warm compresses, and antibacterial bath protocols.
Antibiotics if used wisely and prescribed properly can be a necessary part, and sometimes a life-saving aspect of treating these infections. It is my wish to impart upon you a more thorough knowledge of the pros and cons of each type of conventional treatment approach.
It is also my opinion (and that of many professionals), antibiotic therapies should only be used for more urgent or life-threatening situations, largely due to the growing problem of antibiotic resistance and that these drugs carry a significant personal health risk. This is where alternative therapies shine. Click here for a review of alternatives treatments for Staph and MRSA
Below are summaries of many of the conventional, mainstream or allopathic medicine approaches that are currently available for MRSA and Staph infections. This summary discusses the basic nature and important considerations of each individual method. An important note is that antibiotics for Staph do not always work for MRSA.
Warning: If you are pregnant, or if you have any questions regarding the use of any method for handling MRSA or Staph infections or any other medical condition (for you or someone else), or for details on precautions you should take, do your own research and speak with a qualified health care practitioner.
The most common conventional therapies
- Antibiotics – Antibiotics are drug products that stop or inhibit the growth of bacteria and are often prescribed for MRSA and Staph. They were first synthesized in the 1930’s and have been used extensively since then. There are many different classes and types of antibiotics that work in different ways, have different characteristics and have limitations on how they can be used. “Broad spectrum” antibiotics work against many different kinds of bacteria whereas “narrow spectrum” antibiotics only work against certain specific organisms.
Antibiotics are typically prescribed for internal infections which can include bacteremia, endocarditis, pneumonia, bone, joint and prosthetic infections, surgical site infections, bladder and central nervous system infections. They also may be prescribed for skin infections and for nasal decolonization.
Click the link to find out more about antibiotics for Staph.
Click the link for more about MRSA antibiotic treatments. - Warm Compresses – Warm compresses are often used to bring a boil or abscess to a head and allow it to drain on its own. A washcloth wetted with hot water can be laid over the boil over several days to achieve this. Topical antimicrobials are often used along with warm compresses.
- Incision and Drainage – Boils and abscesses are often incised or lanced by a doctor and drained to reduce pain and to decrease the number of bacteria in the infected area. The procedure consists of treating the skin with a topical antiseptic followed by puncturing or opening the skin with a sterile instrument thus allowing the pus to drain out. Lancing and draining must be done by a health care professional due to the very high risk of spreading the MRSA internally to your blood stream, to other parts of the body or to other people. Secondary infections and other complicating problems can occur if the procedure is not done properly.
- Topical Antimicrobial creams and ointments – Topical products containing antimicrobial agents are often used to manage MRSA infections and Staph infections of the skin. These antimicrobial agents typically kill the bacteria or prevent them from growing. Some commonly used topical antimicrobials include Iodine and Chlorhexidine (Hibiclens). Antibiotics such as Bactroban (mupirocin) are often used in topical antimicrobial products as well. Topical antimicrobials are typically spread or sprayed into a skin infection.
Side Effects: Bactroban should not be used if you are breastfeeding. Topical antimicrobial Chlorhexidine (Hibiclens) is a synthetic antimicrobial to which some people can acquire skin sensitivity. Studies also show that MRSA may become resistant to chlorhexidine over time. Topical antimicrobials likely upset the balance of “good” bacteria on the skin (normal skin flora) which protect your body from infection. This can increase the risk of re-infection. This is also a harsh product on your skin which can cause dry, cracked skin – an optimal entry for MRSA or Staph to cause infection. Again, as with any antimicrobial, fungal overgrowth in the body can occur with use. - Antimicrobial Baths – Bathing in water containing an antimicrobial agent or disinfectant is sometimes prescribed by doctors for skin infections. Commonly prescribed bath additives are chlorhexidine (Hibiclens) and bleach (Clorox). Bleach baths may be less effective at killing MRSA than normal Staph bacteria and antibiotic resistance is a growing concern for chlorhexidine.
Side Effects: Bleach can be harsh and sensitizing to the skin, especially with repeated use. Chlorhexidine should not be used if you are pregnant or breast feeding. The skin has a very large surface area and readily absorbs bath additives into the body. Therefore, the effects of absorbing synthetic antimicrobial agents and harsh chemicals on the body’s immune system should be considered. Additionally, these harsh chemicals often cause skin sensitivity, and dry, cracked skin. Your skin is your first line of defense against Staph and MRSA bacteria. Bacteria can penetrate cracked skin much easier.
Why modern medicine often fails when it comes to recurring infections
It’s important to realize that conventional medicine approaches any disease, including Staph or MRSA, as an isolated event, confined to a specific area in which it resides (like a skin infection, eye infection, lung infection, etc). The solution is usually sought through surgical and/or pharmaceutical drugs.
Seeking to understand WHY the infection appeared in the first place is usually not explored. The focus is usually on the symptoms of disease rather than the root cause. This is a very important concept because conventional medicine suffers when it comes to recurring infections. This is because there is often a much larger issue going on aside from the symptoms of infection itself, and without addressing the entire picture, the infection keeps returning.
The benefits of modern medicine certainly come into play for trauma and surgery. You don’t call your herbalist if you break your leg. And, good Infectious Disease (I.D.) doctors, along with proper culture tests, can help you identify the source of your infection (what type of bacteria) and what antibiotics the bacteria are sensitive to (what antibiotic will work).

Please note: I am a Microbiologist and Scientist. I am NOT a doctor or health care professional. The commentaries above are based upon my personal research, sometimes my own personal experience, historical data, and other people’s experiences with MRSA or Staph. The list of methods above is by no means complete.
Be sure to educate yourself on the many natural antibiotics that Staph and MRSA are not resistant to. An informed person is an empowered person, more able to control their health and achieve long-term success with their infection. Learn more about conventional versus alternative approaches and their pros and cons.




