MRSA Antibiotic Treatment Overview
Updated October 13, 2025
Antibiotics are commonly prescribed as a treatment for MRSA skin infections, either by themselves or along with draining of the infection by a healthcare professional.
Antibiotics are also the standard medical therapy for internal MRSA infections. Antibiotic therapy is often prescribed for the following types of infections:
- Skin infections, such as boils or abscesses, that do not respond to incision and drainage
- Systemic or internal infections such as bone, implant or lung infections
- Severe local symptoms
- Severe internal infections that require surgery to remove infected areas
- Immunosuppressed or immune-compromised people
Because MRSA is becoming more resistant and antibiotic treatments often fail, treatment may require newer antibiotics such as the glycopeptides (e.g., vancomycin) or oxazolidinones (e.g., linezolid/Zyvox). Unfortunately, there are newer strains of MRSA that are becoming resistant to these two drugs. When it comes to antibiotics, the list of what works for MRSA is growing shorter each year.
Doctors don’t often discuss the many antibiotic side effects (more below), and what to expect when it comes to dealing with MRSA (read more here). There are also alternative treatments available which can be used alone or in conjunction with antibiotics to help improve your chance of success.
Top 5 MRSA Antibiotic Therapies for Skin Infections
MRSA is now resistant to many types of antibiotics.
Below are five of the most commonly prescribed antibiotics for community-acquired MRSA (CA-MRSA) skin and soft tissue infections.
Note: For drainable abscesses, incision and drainage (I&D) is the first step. Antibiotics are added based on infection severity, recurrence, and patient risk factors.
1. Trimethoprim-Sulfamethoxazole (TMP-SMX, Brand: Bactrim, Septra)
While not FDA-approved specifically for MRSA, laboratory and clinical evidence show that most community-acquired MRSA (CA-MRSA) strains remain susceptible to TMP-SMX. It’s often used for skin and wound infections, abscesses, and other soft-tissue infections, and occasionally for urinary or lung infections when MRSA is confirmed or suspected.
- Side Effects and Precautions: Not recommended during the third trimester of pregnancy or for infants under 2 months old. Possible side effects include mild allergic reactions, rash, fever, or diarrhea. Rare but serious reactions can include low white blood cell counts (myelosuppression), kidney issues, or liver inflammation.
2. Tetracyclines (Doxycycline and Minocycline)
Tetracyclines are among the most common oral options for mild to moderate MRSA skin and soft tissue infections, especially those acquired in the community (CA-MRSA). Both doxycycline and minocycline are generally well tolerated and have relatively low risk for C. difficile infections compared with other antibiotics.
- Side Effects and Precautions: Not recommended during pregnancy, breastfeeding, or in children under 8 years old due to potential effects on teeth and bone growth. Doxycycline can increase sun sensitivity and sometimes causes nausea or diarrhea. Minocycline may cause dizziness, headache, or skin discoloration with long-term use. Serious side effects are rare but can include allergic reactions or liver inflammation.
3. Clindamycin
Clindamycin has long been used for mild to moderate MRSA skin and soft tissue infections, such as boils, cellulitis, and smaller abscesses. When MRSA is confirmed susceptible (D-test negative), it can still be an effective oral or IV option. A D-test checks for hidden or “inducible” resistance to clindamycin — if it’s positive, clindamycin should usually be avoided.
Clindamycin is no longer recommended for deep or invasive infections such as bone or joint infections due to poor penetration and increasing resistance.
- Side Effects and Precautions: The most important caution with clindamycin is its high risk for causing a C. difficile infection, a serious gut complication that can occur during or after antibiotic treatment. You can learn more about this risk in our guide: Top 5 Antibiotics That Trigger C. diff Infections.
- Other possible side effects include diarrhea, nausea, abdominal cramps, or rash. Because of its risk profile, clindamycin is typically reserved for patients who cannot take other MRSA antibiotics or when sensitivity testing confirms it’s still effective.
4. Linezolid (Brand Name: Zyvox)
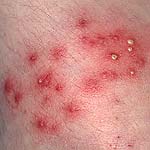
Folliculitis is a common type of MRSA skin infection often treated with oral antibiotics.
Linezolid is an oxazolidinone-class antibiotic that’s highly effective against MRSA, including both community (CA-MRSA) and hospital-acquired (HA-MRSA) strains. It can be taken orally or by IV and has excellent tissue penetration, making it useful for skin infections, pneumonia, and certain bone or joint infections when other drugs are not effective or tolerated.
Because of its cost, and the potential for serious side effects with long-term use, Linezolid is usually reserved for more complicated MRSA infections or when other standard treatments, such as clindamycin, doxycycline, or TMP-SMX, can’t be used or have failed.
- Side Effects and Precautions: Short-term use is generally well tolerated, with side effects like diarrhea, nausea, or headache. Longer courses (typically beyond 2 weeks) can cause bone-marrow suppression, low platelets, nerve damage (neuropathy or vision changes), and lactic acidosis. Linezolid may also interact with certain antidepressants (SSRIs/MAO inhibitors), so medication review is essential.
- Unlike many broad-spectrum antibiotics, Linezolid has a relatively low risk of causing C. difficile infection, but any antibiotic can increase risk in susceptible individuals.
5. Mupirocin – Topical ointment (Brand Name: Bactroban)
Mupirocin is a topical antibiotic ointment used for minor skin infections and to reduce or eliminate MRSA colonization in the nose (see MRSA carriers). It’s often used before surgery to prevent MRSA-related wound infections and may be part of decolonization protocols for healthcare workers or patients with recurrent MRSA.
Mupirocin is for topical use only — it is not effective for deep or systemic MRSA infections and should be used as an adjunct, not a replacement for oral or IV antibiotics when those are needed.
It’s commonly prescribed for adults and children. Limited data are available on its safety during pregnancy and breastfeeding.
- Resistance: Reports of mupirocin-resistant MRSA strains have been increasing, especially with prolonged or repeated use, so it’s best reserved for targeted decolonization or small localized lesions.
- Side Effects and Precautions: Possible reactions include local irritation, rash, burning, or itching at the application site. Overuse may lead to secondary infections, including fungal overgrowth. Systemic side effects are rare due to minimal absorption.
Summary
This list reflects current IDSA (2023) recommendations for oral and topical therapy of CA-MRSA skin infections, including TMP-SMX, doxycycline/minocycline, clindamycin (if D-test negative), and linezolid as systemic options, with mupirocin as a topical/decolonization adjunct.
Top 4 Antibiotic Treatments for Internal or Severe Infections
Hospitalized patients with more complicated or invasive MRSA infections often require intravenous therapy. These infections can include deep soft-tissue infections, surgical wound infections, major abscesses, implant-associated infections, and lung involvement.
Empirically, broad-spectrum antibiotics may be used initially (pending culture results) and then narrowed once MRSA is confirmed. A PICC line may be used for prolonged IV therapy.
1. Intravenous (IV) Vancomycin
A mainstay for serious MRSA infections. Although still widely used, resistance and treatment failure have been reported. Therapy often lasts weeks to months. Its tissue penetration is variable, and bone penetration can be limited in some settings. Used in MRSA pneumonia, bloodstream infections, and deep-seated MRSA infections.
Vancomycin requires IV administration into a vein and can occasionally have severe side effects.
- Resistance: Some strains of MRSA are now becoming resistant to Vancomycin, with one strain called “VRSA” (Vancomycin resistant Staph aureus).
- Side Effects and Precautions: Can cause kidney stress (nephrotoxicity) and, rarely, hearing problems. Rapid infusion may lead to “red man syndrome” (flushing, rash, itching). Other possible side effects include nausea, low blood pressure, or diarrhea. As with many antibiotics, secondary yeast or gut infections can occur.
2. Oral or Intravenous (IV) Linezolid (Zyvox)
Used when IV agents are not feasible or when switching to oral therapy. Has excellent tissue distribution, including lungs and skin. Often reserved for cases where vancomycin or daptomycin aren’t suitable.
- Side Effects and Precautions: Usually well tolerated for short courses, but prolonged use (over 2 weeks) can cause low blood counts (anemia, low platelets), nerve damage (tingling or vision changes), and interactions with antidepressants (SSRIs). May also trigger mild nausea, headache, or diarrhea.
3. Intravenous (IV) Daptomycin
Approved for MRSA bacteremia, right-sided endocarditis, and complicated skin/soft tissue infections. (Note: not used for pneumonia — inactivated by lung surfactant.)
- Side Effects and Precautions: Can sometimes cause muscle pain or weakness (myopathy) and elevations in a muscle enzyme called CPK — doctors often monitor blood levels during treatment. Other possible effects include rash, constipation, or mild dizziness. Not used for pneumonia because lung surfactant inactivates it.
4. Oral or Intravenous (IV) Clindamycin
Though primarily used in skin/soft tissue cases, clindamycin may still be considered in selected internal infections when sensitivity is confirmed and the strain is susceptible. It is far less commonly used as sole therapy for invasive MRSA now.
- Side Effects and Precautions: The biggest concern with clindamycin is C. difficile infection, a serious antibiotic-associated colitis that can occur during or after treatment. Other possible effects include nausea, abdominal cramps, diarrhea, or rash. Should only be used for MRSA when the strain has been tested and confirmed sensitive.
Summary
These details come from the latest 2023 IDSA treatment guidelines and FDA safety information on MRSA antibiotics.
Support Your Gut While Treating MRSA

Antibiotics are often needed to clear a MRSA infection — but they can also disrupt the balance of healthy bacteria in your gut. This imbalance may lead to digestive issues, diarrhea, or even recurrent GI infections down the road.
Supporting your microbiome during and after antibiotics can make a big difference. RestorFlora combines Saccharomyces boulardii and spore-forming Bacillus probiotics that help protect your gut during antibiotic use — without being destroyed by the antibiotics themselves.
Once your antibiotic course is done, MegaSporeBiotic can help recondition your gut microbiome and support a healthy immune balance.
Together, these science-based probiotics can help keep your gut strong while you heal — and may lower the chances of digestive upset or post-antibiotic issues like C. diff.
These professional-grade supplements are available from Michelle Moore’s Embrace Health Naturals store, where you’ll also find personalized guidance and support.
What’s the Best Antibiotic for MRSA?

Finding the right antibiotic. If you think you have MRSA, talk with your doctor about getting tested to help see which antibiotics could actually work against your particular infection – click here for more about testing.
What’s best for you? The antibiotic your doctor may prescribe can vary due to the location of your infection, severity, your health status and if you have allergies to any antibiotics. So keep in mind that the information on this page is not all-inclusive, nor is it meant to imply that any of these drugs are safe or effective options for you.
About side effects, drug interactions and things to avoid with these drugs. Many things can weaken the effects of some antibiotics, and some things don’t mix well with these drugs. You’ll get the most benefit from antibiotics by knowing how to use them properly, safely and effectively. The info on this page is abbreviated and does not include all possible side effects, interactions and contraindications. So be sure to talk with your doctor about your medications and look at the drug product insert for a complete listing side effects, possible drug or food interactions and precautions.
Which Antibiotics Should You Avoid?

MRSA is inherently resistant to many antibiotics, especially those in the β-lactam (penicillin/cephalosporin) class, including methicillin, penicillin, and amoxicillin.
First-generation cephalosporins (such as cefazolin, cephalexin, cephalothin) are effective against MSSA but generally ineffective against MRSA.
In rare cases, reduced susceptibility to vancomycin (VISA or VRSA) has been observed, but this remains an uncommon phenomenon in typical MRSA infections.
Other antibiotic classes that should be used cautiously (or avoided) for MRSA include:
- Fluoroquinolones (e.g. ciprofloxacin, levofloxacin): MRSA rapidly develops resistance to this class, and these drugs carry high risks for C. difficile infection and MRSA colonization due to disruption of normal flora. They can also cause serious side effects such as neuropathy, tendon injury, and lactic acidosis during prolonged therapy.
- Macrolides (e.g. erythromycin, azithromycin): MRSA strains are frequently resistant, and these can also increase gut imbalance and C. diff risk in some patients.
Because of these resistance patterns and safety issues, these antibiotic classes are not considered reliable or preferred treatments for MRSA infections.
Independent Side Effects Listing. RxISK.org is a free, independent drug safety website where you can research your antibiotic for ALL of the side effects that actual people are experiencing. You can also report your side effects. Click here to go RxISK.org.
What Other Options Are There?
Unfortunately, MRSA continues to develop resistance to more antibiotics each year. Even the CDC has warned that it’s only a matter of time before some infections can no longer be reliably treated with standard antibiotics.
In addition, many people struggle with antibiotic side effects or relapse soon after finishing treatment. After several failed rounds, it’s understandable to look for safer and more sustainable options.
Fortunately, there are natural and alternative therapies that can complement or, in some cases, replace antibiotics—without many of the side effects or resistance problems. Learning about these approaches can help you work with your healthcare provider to choose the safest and most effective path forward.

- Natural and Alternative Remedies for MRSA and Staph – Options with fewer side effects and minimal resistance
- Why MRSA Testing is So important? How proper testing can guide your treatment and reduce relapse.
- Top 5 Antibiotics That Trigger C. diff Infections Understand which drugs carry the highest C. diff risk.
- What Your Doctor Might Not Tell You About MRSA Learn what questions to ask before starting antibiotics.
References
1. Liu C et al. Clinical Practice Guidelines by the Infectious Diseases Society of America for the Treatment of MRSA Infections in Adults and Children (IDSA MRSA guideline)
2. CDC outpatient management of MRSA skin infections (MRSA SSTI flowchart)
3. Tong SYC et al. Staphylococcus aureus Infections: Epidemiology, Pathophysiology, Clinical Manifestations, and Management. Clin Microbiol Rev.
4. Brown KA et al. Antibiotic Prescribing Choices and the Risk of Clostridioides difficile Infection. Clin Infect Dis. 2021.
5. Zhang J et al. Comparative Risk of Clostridioides difficile Infection With Commonly Prescribed Antibiotics in Outpatient Settings. Antimicrob Agents Chemother. 2022.
6. Rybak MJ et al. Therapeutic Monitoring of Vancomycin for Serious MRSA Infections: A Revised Consensus Guideline. Am J Health-Syst Pharm. 2020.







